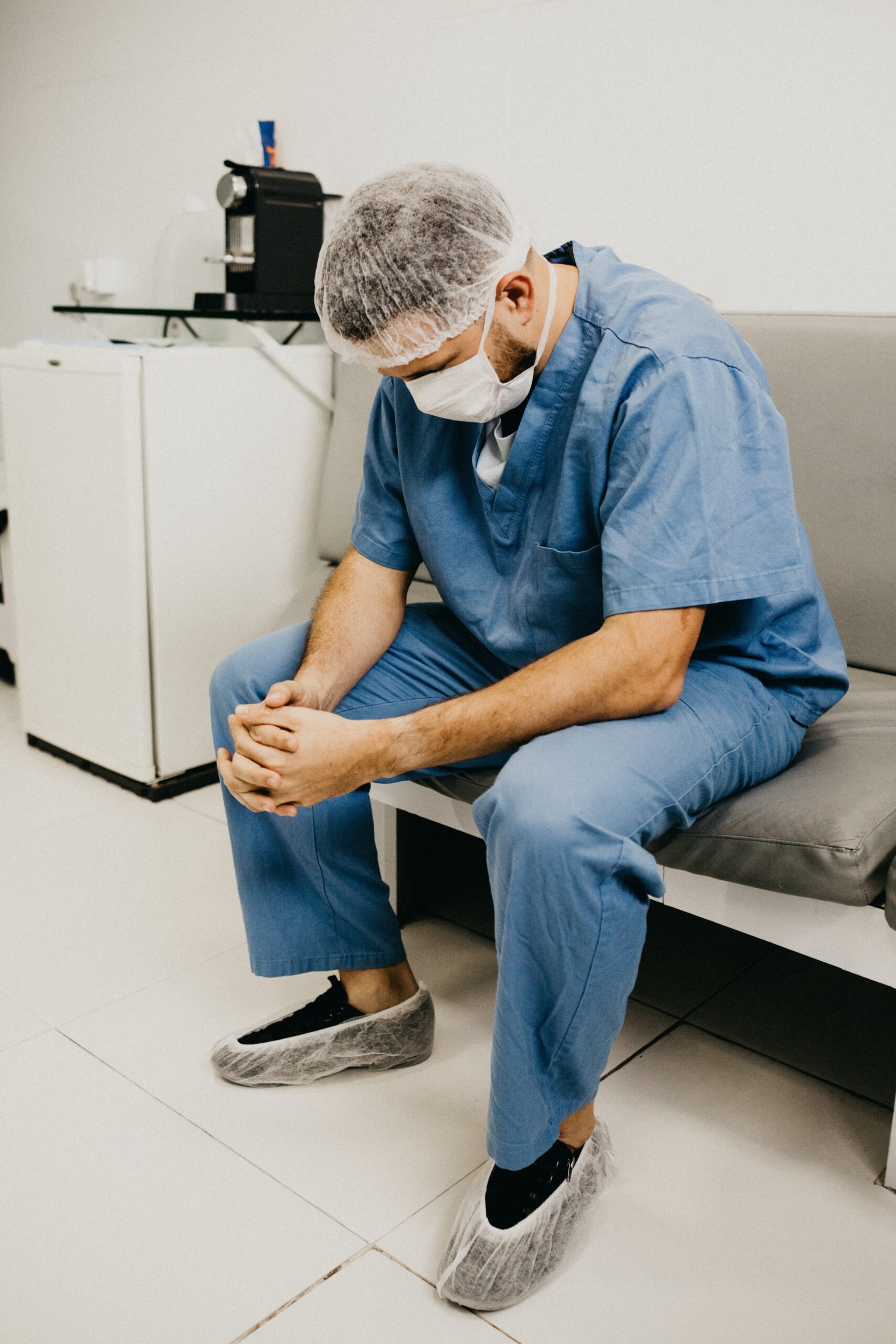
Arabella Kurtz shares lessons learnt during the pandemic providing psychological support to health and social care colleagues.
I am a consultant clinical psychologist and psychoanalytic psychotherapist with longstanding interests in the needs of healthcare staff and reflective practice. In early 2021 I led set up of a psychological support service for health and social care staff in Northamptonshire, one of 41 mental health hubs commissioned at speed by NHS England in response to the pressures of the pandemic. We built a team of eight psychologists, and have now worked with 735 individuals and 81 teams. In this article I’m going to reflect on lessons learnt and what their relevance might be to the legal profession.
Removing barriers to access
We made every effort to remove barriers to using the service, knowing that medical colleagues, used to focussing on the needs of others, find it hard to seek help for themselves. Colleagues referred themselves via a quick online form, and we pretty much did away with suitability criteria. We invited colleagues to come to us with anything, whether it was work-related or not, and however big or small it seemed to them. We got back to them within 2 days and offered a first appointment within a fortnight; we also operated a highly confidential service with a separate record keeping system – away from the general and occupational health record.
This had the desired effect: the service was in great demand from the start, and unexpectedly large numbers of senior colleagues referred in. Those in leadership positions told us how important it was to be able to ask for help without anyone knowing about it. I imagine lawyers to be similarly reluctant, particularly senior lawyers, visible in their firms and accustomed to being the ones others come to for expert advice.
Highly trained professionals on the frontline
We offered psychological consultations at point of referral – up to four hour-long sessions – rather than therapy as such. In essence what we provided was rapid access to trained and experienced mental health professionals – a reversal of the stepped care model, where assessment is followed by a wait for treatment and first contact is usually with more junior practitioners.
Evaluation of service model
We evaluated our model, and it proved highly effective. We used the Warwick-Edinburgh Wellbeing Scale to measure outcome: the average positive shift in scores was 13.7, three points above what is classified as ‘meaningful change’, and there was a fivefold increase in those who reported a positive sense of wellbeing. We referred onto other services in only 11% of cases, which was considerably less than expected. We also had a big impact on sickness rates: 58% referring in were off sick or at high risk of going off sick; after consultation 70% of this group were back at work or no longer at risk of going off sick. This was unexpected because our agenda was not to get people to stay in jobs or return to work, but to provide a real focus on them and their wellbeing. Paradoxically, this seemed to improve staff retention.
I have become firmly convinced of the value of putting highly trained professionals on the frontline and the false economy of the stepped care model, which underpins many of the employee assist programmes marketed to law firms. I would urge legal colleagues to consider paying more to buy in high quality mental health services for staff, or at least to make sure they know about the difference between what is on offer from those with widely varying levels of mental health training and experience.
Personal and work problems interrelated
We learnt early on there was little distinction between personal and work problems – family life was impacting enormously on colleague’s ability to function at work and vice versa. I am sure these reciprocal influences are very similar for lawyers, even if they are not spoken about as openly as they might be. We also learnt about the power of vocation in healthcare to help and hinder: for many personal identity was closely bound up with work, motivating and giving them purpose, but costing them dear when tasks became overwhelming or impossible.
Teams and impact of work environment
Another important lesson was on the impact of the work environment, especially the team environment, on the mental health of colleagues. Psychological problems are often viewed as the responsibility of the individual and wider social and environmental influences are overlooked or underestimated. We often heard that being in a good, supportive team was what made colleagues want to come to work and kept them going when things got tough, and, conversely, could be the decisive factor in quitting. We heard about badly designed jobs, unsustainable workloads and highly distressing team dynamics.
As a result, I’ve developed a strong interest in how to support teams and improve team culture, which begins with identifying and overcoming barriers to the investment of time and resource in relationships at work. Psychological support for managers in supporting their teams is now part of our offer, alongside direct work with teams – facilitating reflective practice, or thinking about how to clarify roles and team structures.
I could go on – it’s been an incredibly difficult time, but the pace of learning and development in these new psychological services in health and social care across the UK has been enormous. It would be wonderful to be able to make use of these innovations in the legal sector.
Let Arabella know what you think
- What in this article is of most interest to you?
- What should we be doing to look after the mental health of lawyers?
Email [email protected] or comment on any of our social media posts about Arabella’s article.

More about the author
Dr Arabella Kurtz is a consultant clinical psychologist and psychoanalytic psychotherapist and leads the wellbeing service for health and social care staff in Northamptonshire. She has held posts in NHS adult and forensic mental health services, and on the clinical psychology training course at the University of Leicester. She has authored two books (‘The Good Story: Exchanges on Truth, Fiction and Psychotherapy’, Viking 2016, together with novelist J.M. Coetzee; and ‘How to Run Reflective Practice Groups: A Guide for Healthcare Professionals’, Routledge 2020) and a number of chapters and research papers.
We're here to listen…without judgement
Contact our free, confidential, emotional support service for the legal sector
Sign up to our newsletter to receive regular support, tips guidance and news on mental health in the law sector.
"*" indicates required fields